It never stops amazing me how quickly time can pass. Two months from now will mark the 3rd year since my test results came back positive for Lyme Disease and Bartonella, and three months after that I began treatment under the care of an Infection Disease Specialist using IV antibiotics through a central line. This lasted for a year and a half, and on the 506th day they removed my central line. It was such a liberating sensation; I could shower without plastering Gladd Press N Seal all over my chest, I could swim and change my shirt without worrying about snagging and pulling the line – I’d become free. At this point I had decided I no longer wanted to take antibiotics any longer (you can read about it in this post) and in January of last year I travelled to a biological medicine clinic in Switzerland called Paracelsus. I am so happy to tell you I’ve been antibiotic free for 13 months. In August 2018 I travelled back to Paracelsus and it has been interesting since then with (as always) with more tests of faith, and also triumphs. If you’re just finding these blogs, you can head into the archives and read about my journey from diagnosis to treatment, both on antibiotics and my daily journals from my time at Paracelsus.
Coming home from Paracelsus the second time was a whirlwind.
During treatments on my last day at the clinic I had my second, and final DMPS infusion to help remove heavy metals. I’ll be doing these at home too, but during my last appointment with the doctor (after the infusion) my head hurt like something fierce. I thought I needed food, but despite my effort to eat a substantial lunch my headache didn’t improve. Within a few hours my headache became worse, I laid in bed with my eyes closed and tears escaping my eyes. Stephen, amazing as always, noticed my forehead had become warm, so he put a cold cloth on my head and I napped for a couple hours.
I woke up in the morning with a stiff neck, so bad it completely limited my ability to turn my head side to side. This was our last day in the country and we took a drive with Stephen’s grandma. By dinner time we visited his Uncle’s and my neck had gotten much worse. We stayed a little later than I should have considering we had to get up early to fly home. When I woke the next morning, I was in so much more pain with my neck and definitely not looking forward to traveling home.
It took 14 hours and two flights before we arrived to the hotel. By then it was clear something was wrong, and despite being sore and tired himself Stephen tried to help me out by heating facecloths, placing them on my neck and massaging it. The problem was that even the slightest touch hurt. A lot. The kind-of-hurt that makes you gasp, cringe and reflexively pull away. For the next three nights I slept with one of those travel U-shaped pillows to stabilize my neck and keep it from moving and causing pain.
After three nights at home we had to leave town again. My insurance company sent me to a doctor in Southern Ontario. We flew right from our small town, which was nice–saving us a four hour drive each way before getting on another airplane. Altogether we were out of town for about 36 hours.
When we arrived in the Toronto area and got to the hotel, all I could do is lay on the bed with tears running down my cheeks while I breathed through the pain. It felt like my fire mixed with my blood scorched its way through my veins.

our local airport
The next day we saw the doctor. The visit was upsetting for me, so I won’t to go into a lot of detail. The appointment lasted for one and a half hours with a lot of dialogue. I was still in pain while I sat there, but like I always do–I tried to be tough and get through the appointment the best I could.
During the appointment I had to bite my lip from time to time. I didn’t do it to keep myself from saying anything, rather it was to keep the tears from coming. I needed a distraction and causing myself pain seemed like the only distraction I could come up with. The doctor talked about the how the priority needed to be ruling out life-threatening illnesses; he listed most of the ones we’d crossed off a couple years ago, but he left the thought unfinished.
With all that talk of life-threatening illnesses it brought me back to 2015 and then my brain got the best of me, I sat there wondering,
“Oh $h!+, am I dying faster than ‘normal’ right now? Did we miss something?”
It is a terrifying thought. It time warped me back to the end of 2015 and beginning of 2016 when I laid in bed wondering how long I’d live, accepting that whatever was happening might claim me. The only way I could stop listening and block out the conversation was to bite my lip as hard possible without being too obvious.
The doctor discussed a lot of his thoughts with us and talked about a few scenarios that related to the treatment I’ve had over the last couple years. Ultimately he said,
“life isn’t a movie with different plot lines, maybe you would have got better anyway–and that you made these improvements despite the antibiotics, not because of them”
Anyway, in my attempt to keep this short and in order to not relive the entire appointment I will stop it there. When I walked out of that appointment I sat on the bench outside while we waited for the taxi and I cried. I didn’t cry because of the things the doctor said. I cried because I brutally realized the intention of the appointment was not to help me. The doctor’s goal was not to help find a different diagnosis, or treatment plan, or come up with a plan to improve my quality of life. The only intended outcome was his report to the insurance company.
It dawned on me: I didn’t see a doctor whose goal was to help the suffering.
His report was shared with my family doctor and it offered a few suggestions, but nothing that helped in my treatment, recovery or to improve my quality of life. But it was at least a bit of extra insight we could use.
I’ve been lucky to have had many doctors who’ve cared so much you can read it on their face. Those doctors are the ones who matter, and will always have a place in my heart because these are the ones who go above and beyond what we’d ever expect.
By the time we got home it was mid-September, and I continued with my weekly IV infusions from Paracelsus. I still had four unused infusion sets from my previous treatment plan so I used those up first but we ran into difficulty. Over the next few weeks accessing veins became much more difficult. My veins were often collapsing, or if we got a catheter in, by the second day it would float out of the vein. By mid-October I had used the old infusion sets up and started into my new treatment plan: three infusions per week that consist of a build-up infusion, procaine infusion and detox with DMPS for removing heavy metals. Despite having done the DMPS infusion twice at Paracelsus it did not go well for me at home for the first time.

some of the meds from one of my infusion sets
I ended up in bed for a week after the infusion and had lingering symptoms for a couple weeks after that. The idea with doing the DMPS infusion is that it should pull out the heavy metals (you can see the results of my heavy metal test in this post) and ideally your body will then excrete the metals. However, if the body isn’t able to clear the metal fast or well enough, it will reabsorb them and can cause issues. They think this is what happened.
What was doing the DMPS infusion like?
Midway through the infusion I got sharp stabbing pain in my head behind my eyes. By the end of the infusion I wasn’t able to sit up and get off the couch on my own because of sudden weakness and in a flare of intense neurological pain that lasted for days. It was the worst in my arms and legs, which severely affected my sleep. For me, pain like this feels like someone is stabbing me with hot knives. Laying down had been the only option over the next few days, and even that hurt. Have you ever gone camping or had a sleepover when you were young and you slept on the ground? Then woke up because your hip bone or tailbone was digging into the ground and had gone numb and painful? This was the feeling I had in my legs all night long. It would stop for a five to ten minutes once I shifted my body, but even to do that took a painful effort.
Almost any of the symptoms I ever had flared up at this point. My joints felt like they were splintering apart. I had a week long fever, and a few nights I would wake and have to change into new PJs because I sweat through the original ones. I read and slept a lot through the first five days.
If you remember my lasts posts about my time at Paracelsus, you might recall the lumps I got in my wrists, and these had continued since being home and were now more frequent, as in a couple times per week. I can’t use my hands when they’re like this – so it painfully limits what I can do in a day. I also developed strange pockets of swelling on my inner wrists and around my ankles. Apparently things can still become more strange.

painful lumps in my wrists
At this point the doctors told me to hold off on the detox and DMPS IV for a few weeks. In that time I tried to continue with the other two weekly IVs but ultimately my veins failed us. After three weeks of trying multiple times without success, we stopped trying, and they referred me to have a port-a-cath placed.
While taking a break from the detox and DMPS one of my doctors asked me to start a kidney, gut and liver cleanse using the Dr. Clark programs. This was a four-to- five week process, which I finished at the end of November. Throughout this time my symptoms gradually resolved again except the pain in my legs. The pain was wicked at night and I became run down and exhausted. To address the pain, I had to increase my lamictal dose (this is one of my meds that helps control neurological pain). During the cleanse programs I took a high dose of turmeric, a supplement I’d already been taking for a couple years–but the dose had been at least 5 times more with the cleanse. I noticed that it seemed to help with inflammation at a dose that high (1500mg three times daily)–if you’re reading these out of interest in my story, then this doesn’t help much–but I thought if there was another person suffering it might be helpful information. With that said, PLEASE talk to your doctor or pharmacist before adding any new supplements or increasing the dose of anything.
Can I say the DMPS caused the flare?
No. Definitely not. I had been getting flare after flare of joint pain, lumps and swelling for a couple months before the infusion. Flares can come without reason or expectation. If I skip ahead to January when I did another DMPS infusion I still had symptoms after, but all of which had also flared a week or so before I did the infusion. The bright side was that overall, I tolerated it well compared to in October.
So, when people ask how I’m doing all I can say is,
“it is still up and down, but I still feel like I’m moving in the right direction and that progress is (very) slowly being made”
To round out 2018 had a port-a-cath placed which is a blessing as it will help deliver the meds that make a difference for me: my infusions. To take these as prescribed has played a big role in the improvements I’ve made.
On December 7th I went for surgery for the port-a-cath. I was somewhat nervous, but it isn’t too different from the central line I had in 2016/2017. If you’re not sure what a port-a-cath is then a quick Google search will help explain it for you. It’s an implanted device, with a rubber chamber under my chest and that chamber connects to a catheter that goes into a central vein to deliver intravenous medication. To access the port, you use a special needle and poke through the skin into the rubber chamber. From that point once it is in the right position you put a dressing over it and can run your medication. When you’re done with the IV, then you remove the needle and are free to shower, swim or do whatever you like. Having a port means no more poking at my veins and it is so much nicer than the central line I had: the central line is always sticking out of your chest, 24 hours a day, seven days a week.

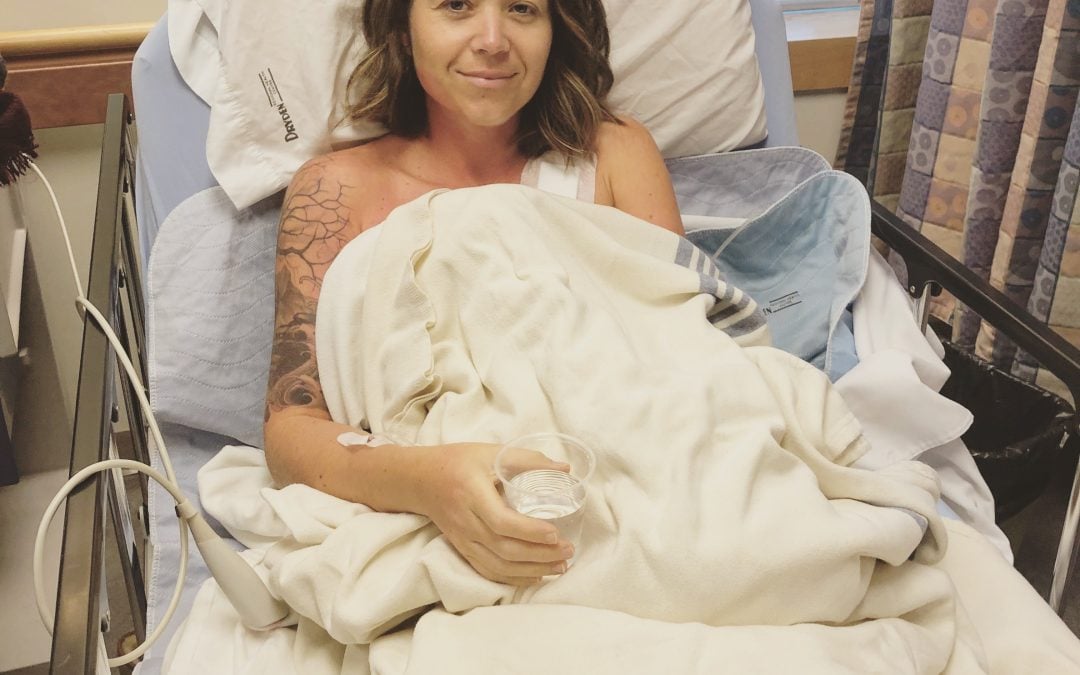
after having the port-a-cath placed (and still groggy)
After four pages I would say post is long enough as it is so I will stop it here and write a separate post about getting the port-a-cath and my first experience with it. This was something I took time to research and prepare myself for, so I think as a separate post it might be helpful to other people who find themselves in a similar situation.



I have lyme myself. After years of antibiotic treatment and hyperbaric oxygen treatment, which I paid for myself, I have probably gotten about 95% of my life back. The problem I am seeing on the West Coast, is that physicians here hardly ever consider lyme as a diagnosis. I see many friends and their relatives who present in much the same way my case did. I think many of these patients actually may have lyme disease. Most aren t even tested for lyme. Most end up with a diagnosis of fibromyalgia. We know that fibromyalgia is a non-diagnosis in the sense that the cause is unknown and the current treatment treats only the symptoms instead of the cause.
That’s so great to hear you got back on your feet! I don’t live anywhere near. HBOT and haven’t committed to buying one, but I did get to try one out this past winter. It gave me a really bad weeklong herx-life affect, which I knew was a possibility. If I had access to one I’d definitely try a few sessions though and see how it went.
Sara, your inner strength will get u through. You are an amazing woman, and loved by all. You got this! Thanks for sharing your journey! Hugs, Carrie
Thanks so much Carrie! <3
Sara thanks for sharing again I pray things will get better for you in 2019 hugs
Thanks Lynne! ☺️❤️